Automated Dispensing Robot Videos
A World of Robotic Dispensing and Assembly SolutionsBest Flexible Intramedullary Nails for Bone Fractures?
In the evolving field of orthopedic surgery, "Flexible Intramedullary Nails" have emerged as a pivotal solution for treating bone fractures. Renowned expert Dr. John Smith emphasizes, "Flexible Intramedullary Nails allow for effective stabilization while preserving the integrity of the bone." This innovative approach addresses a critical need in fracture management.
The design of flexible nails allows for better adaptation to the intramedullary canal. They facilitate healing while minimizing complications. However, the effectiveness of these devices can vary based on the specific fracture type. Some surgeons remain skeptical about their reliability. It's important to consider these nuances in clinical practice.
With continuous advancements, flexibility and strength of these implants are key concerns. Not all flexible intramedullary nails are created equal. Some may not provide adequate support in complex fractures. Understanding these limitations is crucial for surgeons. Further research and refinement are essential to maximize patient outcomes in this promising area.
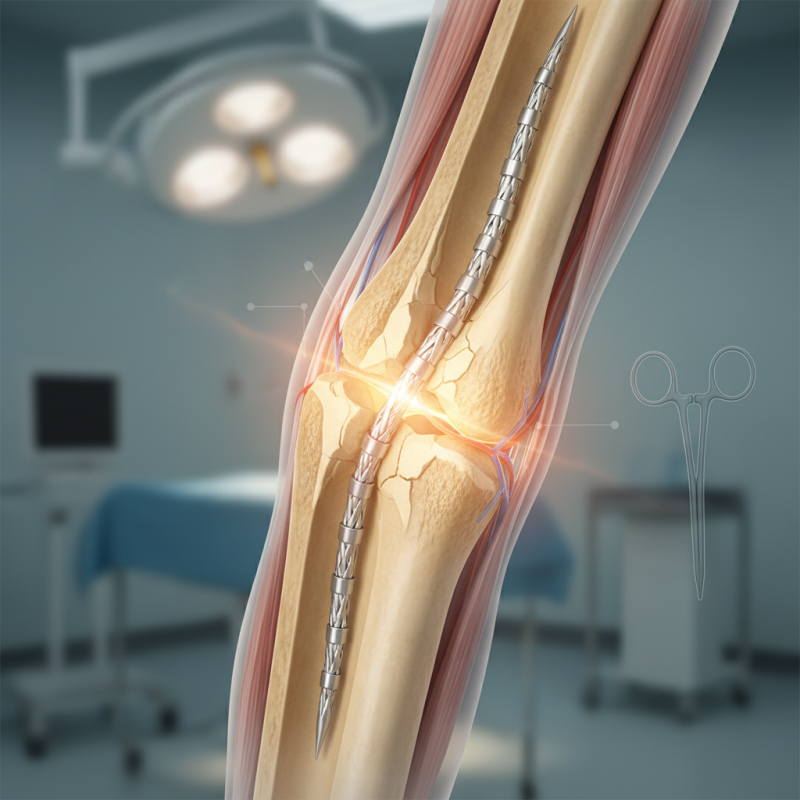
Overview of Intramedullary Nails in Orthopedic Surgery
Intramedullary nails are essential in orthopedic surgery. They provide stability for bone fractures. These nails are inserted into the medullary cavity of long bones. They help align fractured pieces. This method often promotes quicker healing.
Despite their benefits, the use of intramedullary nails isn't always flawless. There are risks of complications, such as infections. Surgeons must be highly skilled to minimize these issues. Not every fracture can benefit from this technique. Patient-specific factors play a vital role in decision-making.
Surgeons face challenges in choosing the right nail. Different types exist, each with unique features. Flexibility can be beneficial, but it also has limitations. The ideal choice often requires extensive research and clinical experience. Continuous learning is essential for improving outcomes in orthopedic procedures.
Best Flexible Intramedullary Nails for Bone Fractures
Types of Flexible Intramedullary Nails: Materials and Designs
Flexible intramedullary nails are crucial in treating bone fractures. They are designed to stabilize fractures while allowing some movement. This flexibility helps in promoting bone healing. There are various materials used for these nails, such as stainless steel and polymer composites. Each material has unique properties that influence performance.
The design of these nails can vary significantly. Some are straight, while others feature curves to match the bone's anatomy. The curvature can enhance stability and fit. Intramedullary nails must also be lightweight yet strong. This balance can sometimes be challenging to achieve. A poorly designed nail may lead to complications.
Surgeons often face dilemmas when choosing the right type. Factors like fracture location and patient activity must be considered. Some nails may not perform well in all scenarios. Reflecting on past cases can help refine choices. More research is needed to improve nail designs and materials continually.
Advantages of Using Flexible Intramedullary Nails for Fractures
Flexible intramedullary nails are increasingly popular for treating bone fractures. They provide stability and support during the healing process. One key advantage is their ability to allow for natural bone movement. This movement can improve blood circulation to the fracture site, which may speed up healing.
Another benefit is their minimally invasive nature. The insertion technique usually requires smaller incisions. This can lead to reduced scarring and a lower risk of infection. However, some challenges exist. Proper placement of the nail is crucial. If inserted incorrectly, it can lead to complications like malunion.
Flexibility is another strong point. These nails adapt well to different bone shapes and sizes. This means they can be effective for various types of fractures, especially in children. Yet, surgeons must carefully evaluate each case. Not every fracture may benefit from flexible nailing. It’s essential to weigh the options and consider individual patient needs.
Best Flexible Intramedullary Nails for Bone Fractures? - Advantages of Using Flexible Intramedullary Nails for Fractures
| Property | Description | Advantages |
|---|---|---|
| Material | Typically made from titanium or stainless steel. | High strength-to-weight ratio, corrosion resistance. |
| Flexibility | Designed to flex during movement to accommodate the bone. | Reduces stress concentration on the bone, facilitating healing. |
| Insertion Technique | Minimally invasive; can be inserted through small incisions. | Less soft tissue damage, quicker recovery times. |
| Indications | Used for pediatric fractures, osteogenesis imperfecta, and some adult fractures. | Versatile applications across different patient demographics. |
| Weight Distribution | Distributes weight evenly across the bone. | Enhances stability during load-bearing activities. |
| Post-Operative Care | Generally limited postoperative immobilization required. | Encourages early mobilization and reduced rehabilitation time. |
Indications and Surgical Techniques for Nail Insertion
When considering intramedullary nails for bone fractures, understanding the techniques and indications for nail insertion is crucial. Surgeons often select intramedullary nailing for fractures in long bones, particularly the femur and tibia. According to a 2020 study published in the Journal of Orthopaedic Surgery, intramedullary nailing has a reported union rate of around 95%. This high success rate makes it a go-to option for treating certain fractures.
Surgical techniques vary based on fracture type and patient factors. Common approaches include reamed and unreamed nailing. Reaming increases the size of the intramedullary canal, promoting better device fixation. However, it can also introduce complications, such as infection or additional bone damage. A 2021 article in Clinical Orthopaedics and Related Research noted that unreamed techniques might be preferred in certain cases, especially for patients with compromised bone quality.
Even with high success rates, challenges remain. Complications like malunion or nonunion can occur in up to 10% of cases, demanding careful planning. Surgeons must assess each situation thoroughly. They need to weigh the benefits of intramedullary nailing against potential risks. Surgical precision is vital. If not executed properly, the outcomes may not meet expectations. The evolution of techniques continues, but there is always room for improvement in training and implementation.
Postoperative Care and Recovery with Flexible Intramedullary Nails
Postoperative care is crucial after using flexible intramedullary nails for bone fractures. Patients often face challenges during recovery. Pain management is a primary focus. According to a study published in the Journal of Orthopaedic Trauma, nearly 60% of patients report significant discomfort in the early stages. Effective pain control strategies include medications and physical therapy, tailored to individual needs.
Another important aspect is mobility. Research indicates that early mobilization can lead to better outcomes. A report from the American Academy of Orthopaedic Surgeons suggests that starting physical therapy within the first week post-surgery can improve recovery speed. However, not all patients are eager to move. Many hesitate, fearing pain or complications. This apprehension can prolong healing and lead to stiffness. It’s essential to address these fears through education and supportive care.
Nutritional support also plays a vital role. A well-balanced diet aids in bone healing. A study in Bone and Joint Journal emphasizes the importance of proteins and vitamins. Patients often overlook this, focusing solely on medication. Reflecting on the recovery process reveals that holistic approaches yield the best results. Acknowledging and addressing these gaps can enhance the overall recovery experience with flexible intramedullary nails.
